What is IBD?
Inflammatory Bowel Disease (IBD) is a general umbrella term referring to conditions that cause chronic inflammation in the gastrointestinal system. The main two conditions that IBD includes Crohn’s disease and ulcerative colitis.
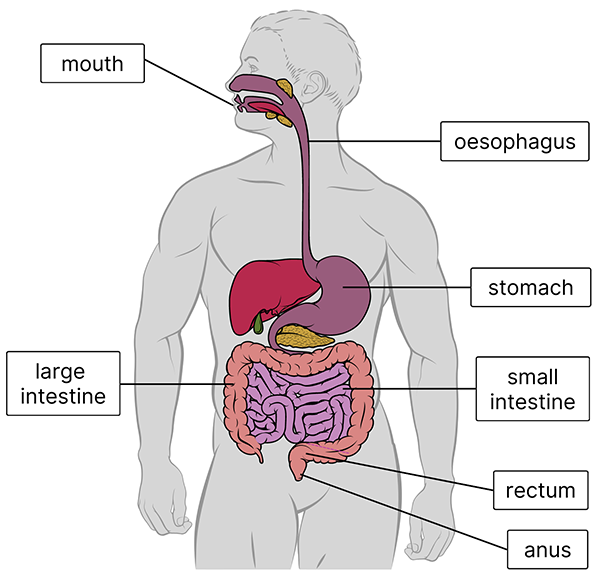
The gastrointestinal system includes:
- the mouth
- the oesophagus
- the stomach
- the large and small intestines
- the rectum
- the anus
The function of our gastrointestinal system is to break down the food and liquids we ingest into substances that the body can use for energy. Undigested material and waste products are then excreted from the body.
When this system becomes inflamed, it is harder to absorb what we need from food, as well as to dispose of waste products. This is why IBD can make people very sick.
Currently, at least 80,000 Australians live with IBD. It is a complicated disease that can vary significantly in severity. While it is possible for this disease to go into remission or for people to have mild symptoms, others experience debilitating symptoms and require hospitalisation or surgery. In some cases, serious complications include malnutrition or colorectal cancer.
All people living with IBD require support and care to manage this disease.
The main types of IBD
Crohn’s disease
 Crohn’s disease is a chronic inflammatory condition, causing inflammation in the digestive system. The small intestine is often the area that is most affected. The lining of the digestive tract becomes inflamed and swollen and penetrates several layers into the lining of the bowel, impacting digestion.
Crohn’s disease is a chronic inflammatory condition, causing inflammation in the digestive system. The small intestine is often the area that is most affected. The lining of the digestive tract becomes inflamed and swollen and penetrates several layers into the lining of the bowel, impacting digestion.
Ulcerative Colitis
 Ulcerative colitis causes chronic inflammation in the large bowel. This inflammation stays on the surface layers of the bowel’s lining and causes small, painful ulcers to form.
Ulcerative colitis causes chronic inflammation in the large bowel. This inflammation stays on the surface layers of the bowel’s lining and causes small, painful ulcers to form.
What is the difference between IBD and IBS?
While IBD and IBS sound very similar, they are not the same.
IBS is a serious condition that can also affect patients’ quality of life. However, IBS is a syndrome that refers to a group of symptoms that frequently occur together. It does not lead to chronic inflammation in the gut, and typically does not lead to hospitalisation or surgery.
There is a wide range of possible causes for IBS, but the risk factors are slightly different. IBS cannot be detected with diagnostic imagery and requires a different investigation for diagnosis.
Because IBS and IBD are unique and require different treatments, it’s important to ensure that you receive an accurate diagnosis.
To learn more about IBS, read our page covering everything you need to know here.
Symptoms
IBD may have a range of debilitating symptoms. One of the most important things to know about IBD symptoms is that they can come and go. When symptoms worsen, it is called a flare-up. When symptoms have improved for several years, patients are considered to be in remission.
However, IBD is often unpredictable and symptoms may even change from day to day. Symptoms may also change depending on the type of IBD you have, and which part of the GI tract is affected. This can make it difficult to understand and cope with the symptoms that you are experiencing. Symptoms include:
- Diarrhoea
- Blood in the stool (this is more common with ulcerative colitis)
- Fatigue
- Weight loss
- Decreased appetite
- Joint pain
- Rashes
- Fever
- Anemia (iron deficiency)
- Stomach cramping and pain
- Bloating and gas
Causes
The exact cause of IBD is still not known, but research has shown that several environmental and genetic factors may increase your chances of developing the disease.
These include:
- Family history. There may be a genetic component to IBD, and you are more likely to be diagnosed if you have a close relative with the condition.
- Smoking. Smoking is a risk factor for developing Crohn’s disease, and increases the risk of complications. Smoking leads to inflammation in the body.
- Age. IBD is typically diagnosed between the ages of 15 and 40.
- Issues with the immune system. Research indicates that the immune system might play a role in the development of IBD. Our gastrointestinal system works with the immune system to protect us from harmful disease-causing pathogens and bacteria that we eat, making our stomach and intestines sensitive to “bad” bacteria or infections.
If an infection or irritant is detected, our gastrointestinal tract will become inflamed to protect us. In IBD, this natural process may become overreactive and the lining of our digestive tract could stay inflamed long after an infection has cleared up.
Testing
There are several diagnostic tests that can be performed to look for IBD. The most common modern tests include:
- A colonoscopy. This involves using a camera inserted into the anus to investigate the bowel for signs of inflammation, damage, ulcers or fistulas.
- A sigmoidoscopy. This is similar to a colonoscopy, but it only examines the final 20 inches of the sigmoid colon (the end of your intestine).
- An endoscopy. An endoscopy involves inserting a camera into the mouth to examine the upper gastrointestinal system for signs of disease.
- A capsule endoscopy. This test involves swallowing a tablet with a small camera inside it, this will take images as it travels through your gastrointestinal system, before it is naturally expelled in stool.
- A biopsy. Sometimes, a small tissue sample called a biopsy may be taken during the above procedures. This can be examined to assist in a diagnosis.
- Imaging. In some cases, your doctor will order imaging tests such as an X-ray, CT scan or MRI.
Due to the increased risk in patients with IBD developing colorectal cancer, your doctor is likely to recommend that you undergo regular screenings for colon cancer.
Treatment
Treatment for IBD will depend on your symptoms and risk factors, as well as the type of IBD you are diagnosed with. Common strategies to treat IBD and manage its symptoms include:
- Anti-inflammatory medication. Anti-inflammatory medicines such as corticosteroids or amino salicylates may be prescribed to reduce inflammation in the gastrointestinal tract.
- Immunomodulators. These are medications that help decrease the body’s inflammatory response.
- Supplements. Supplements such as iron may be given to address nutritional deficiencies.
- Antibiotics. Antibiotics might be prescribed to ensure that there is no infection causing inflammation.
- Laxatives and anti-diarrheal medications. These may be prescribed for symptom flare-ups to moderate bowel movements.
- Surgery. In severe cases, a range of surgeries may be considered to remove or close fistulas, or even to remove inflamed portions of the intestines.

How Moonee Valley Specialist Centre can help
Our empathetic and caring team can provide assessments, diagnosis, and management for IBD. Dr Nathan Connelly is experienced in helping patients with IBD, focusing on providing holistic care to each person.
You will be treated with respect and compassion as we support you with managing IBD.
*All information is general in nature and is not intended to be a substitute for professional medical advice. See a doctor if you experience a persistent change in bowel habits or if you have signs and symptoms of inflammatory bowel disease.

